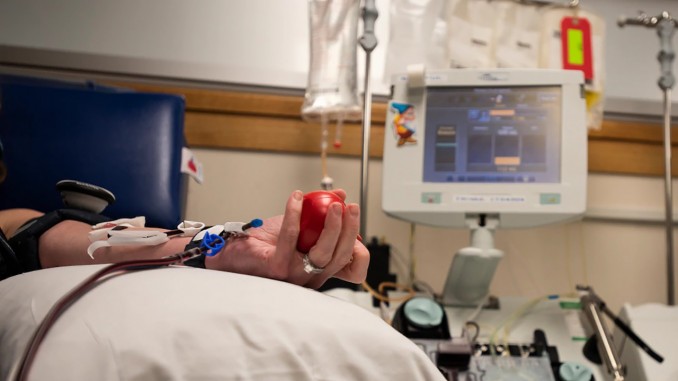
This week the FDA granted Emergency Use Authorization (EUA) for another treatment for patients with COVID-19. This treatment relies on blood transfusions from patients who have recovered from the virus, and thus would have antibodies present in their blood. Since a vaccine hasn’t been developed yet, this is the only way for patients to get actual antibodies that fight the virus.
Currently the U.S. death toll for COVID-19 is over 184,000 people. With no vaccine available, as well as the easing of restrictions, this number will continue to rise in the coming months.
This kind of emergency authorization is only used in cases of dire need, when no other viable treatment exists. It allows the commissioner of the FDA to temporarily approve of medical treatments or drugs that are either unapproved, or are approved for a different use. This is the same authorization that allows the antiviral drug Remdesivir to be prescribed as a treatment for patients in hospitals with severe cases of COVID-19.
A recent study, conducted by the Mayo Clinic and sponsored by the National Institute of Health, showed that treating patients that had severe cases of COVID-19 with blood plasma improved mortality rates. However, this study did not include a placebo group against which to measure this data. This exclusion makes it impossible to determine efficacy rates, and exactly how much this new treatment helps those in need. As Steven Nissen said, a clinical trialist at the Cleveland Clinic, “The lack of high-quality trials in making clinical decisions about how to treat patients with coronavirus infection is a national embarrassment. Here we have another non-randomized study, NIH-funded, and uninterpretable.”
While this could be a promising treatment for patients suffering from the coronavirus, due to the missing data we only know that blood plasma has a potential to save lives, but not that it will. It is irresponsible to tout this as a cure at this point.




